Being an absolute klutz, the risk of lymphoedema really scared me and, before I understood it a bit more, I was convinced I’d get it straightaway. I knew nothing about it before being diagnosed with breast cancer (as if we didn’t have enough to bloody worry about!), but it is an important topic with significant risks, so I had to dedicate a post to it, describing what it is in layman’s terms for any newbies out there and sharing some tales from those who have developed it.
Remember, I’m not a doctor! I’m just repeating info I have been given at various forums and appointments with my LD nurse. Best to have an appointment with a lymphoedema nurse to fully understand your risks and how to avoid it.
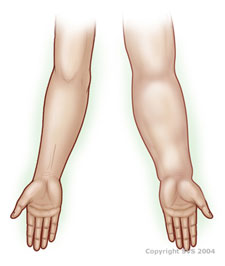 What is lymphoedema? This is when the lymph system can no longer effectively drain certain areas of your body, meaning lymph builds up in the tissue, which then swells up. With breast cancer the most commonly affected areas are your arm, hand and breast on the side on which you were operated as you will have had at least a few of your lymph nodes removed, which may affect the effectiveness of your lymph system.
What is lymphoedema? This is when the lymph system can no longer effectively drain certain areas of your body, meaning lymph builds up in the tissue, which then swells up. With breast cancer the most commonly affected areas are your arm, hand and breast on the side on which you were operated as you will have had at least a few of your lymph nodes removed, which may affect the effectiveness of your lymph system.
What are my risks? Everyone seems to get told different figures when it comes to the risks. My lymphoedema nurse told me about a third of women who had a Full Axillary Clearance (all lymph nodes removed, like me) will develop it, compared to 10% of those who had a Sentinel Node Biopsy (where they remove the first 2 or 3 nodes to test for cancer) – although your risk is increased to that of a Full Axillary Clearance if you have radiation to your axilla.
What can I do to prevent lymphoedema? Prevention is best as there is no cure – if it develops it can only be managed and treated so you then have to learn to live with it. There are a number of things you can do to reduce your risk of getting lymphoedema.
- Avoid cuts, bruises and burns on your at-risk side. Be sensible like wearing protective gloves when gardening, oven gloves when cooking and rubber gloves when cleaning. Also be careful when shaving your armpit and around animals that are likely to bite or scratch.
- Look out for early signs of infection – including redness, warmth, pain and swelling. If you notice anything see your GP immediately who will prescribe antibiotics to keep the infection at bay.
- Always use your other arm for medical procedures like blood tests, injections and blood pressure.
- Do not get a tattoo on your at-risk arm.
- Avoid insect bites – use a strong anti-repellent or wear long sleeves.
- Wear a high sun factor to avoid sunburn.
- Do not lift or carry anything heavy – I was advised no more than 2kg. Particularly difficult if you’re a mum to little ‘uns.
- Avoid straps that dig into your arm, hand or shoulder. This includes handbags, shopping bags and tight bra straps!
- Avoid tight clothes, watches or jewellery that restrict your BC side.
- Avoid extreme temperatures like saunas and steam rooms.
- Do not do repetitive movements for long durations without stopping (like painting or exercising). Take frequent rests and stretch the arm.
- Keep your skin clean and moisturised – clean skin is less likely to develop infection and moisturised skin is less likely to crack.
- Exercise. Following surgery, stick to your physio plan. The gentle stretches keep your joints and muscles working and helps the lymph system develop new pathways to drain the lymph fluid. Once you have recovered, doing other exercise will continue to help your lymph system. I do pilates and swim. Be careful of sports and exercise classes that involve contact that could cause you to harm your arm or involve lifting weights.
- Keep within a healthy BMI range. Being overweight increases your chances of getting lymphoedema – so best to stick to/get to a healthy weight.
- Take some precautionary antibiotics with you if you are going abroad. Your GP should prescribe these for you in case you develop an infection in your arm or breast on your BC side.
- Some lymphoedema nurses recommend wearing a lymphoedema sleeve on long-haul flights.
You can also get medic alert bands and bracelets to wear on your at-risk arm.
 If you DO cut, bruise or burn your arm, or develop an infection, it doesn’t mean you will definitely develop lymphoedema (just as you unfortunately can’t guarantee avoiding lymphoedema even if you follow all of the above and never have an accident). Initially I assumed it was game over as soon as I did anything to the arm. And I am SO INCREDIBLY clumsy that within weeks I’d banged it quite a few times, burned it while cooking and chopped the tip off my finger while chopping onions… Dufus. A month after my final radiotherapy I went on holiday with the intentions to be REALLY good. On the first day, fresh off my long-haul flight, I got sunburnt, bashed into some coral while snorkelling, resulting in cuts and bruises from my wrist all the way up to my shoulder and then topped it off with a couple of mozzie bites in the evening. I thought that was it. Game over. And waited for my arm to swell. Amazingly it didn’t. When I got home I booked an appointment with a lymphoedema nurse to get a better understanding of it all. She measured both arms, all along each arm at 5cm intervals and
If you DO cut, bruise or burn your arm, or develop an infection, it doesn’t mean you will definitely develop lymphoedema (just as you unfortunately can’t guarantee avoiding lymphoedema even if you follow all of the above and never have an accident). Initially I assumed it was game over as soon as I did anything to the arm. And I am SO INCREDIBLY clumsy that within weeks I’d banged it quite a few times, burned it while cooking and chopped the tip off my finger while chopping onions… Dufus. A month after my final radiotherapy I went on holiday with the intentions to be REALLY good. On the first day, fresh off my long-haul flight, I got sunburnt, bashed into some coral while snorkelling, resulting in cuts and bruises from my wrist all the way up to my shoulder and then topped it off with a couple of mozzie bites in the evening. I thought that was it. Game over. And waited for my arm to swell. Amazingly it didn’t. When I got home I booked an appointment with a lymphoedema nurse to get a better understanding of it all. She measured both arms, all along each arm at 5cm intervals and  compared the measurements to see if there was any noticeable difference that could indicate the onset of lymphoedema. Luckily, no evidence of it so far (touch wood – I could obviously develop it at any time). She then showed me a diagram of the lymph system and told me how it works, and explained that some patients never get it as you always have some lymph nodes remaining in that area – either in your chest or under your collarbone – and your body can sometimes work out another way to drain the lymph fluid. But some patients’ internal plumbing means they will definitely get it. So while some people can put their at-risk arm through major trauma with no ill-effects, others can develop lymphoedema with no, or a very small trigger.
compared the measurements to see if there was any noticeable difference that could indicate the onset of lymphoedema. Luckily, no evidence of it so far (touch wood – I could obviously develop it at any time). She then showed me a diagram of the lymph system and told me how it works, and explained that some patients never get it as you always have some lymph nodes remaining in that area – either in your chest or under your collarbone – and your body can sometimes work out another way to drain the lymph fluid. But some patients’ internal plumbing means they will definitely get it. So while some people can put their at-risk arm through major trauma with no ill-effects, others can develop lymphoedema with no, or a very small trigger.
I’m obviously not advocating bashing your arm around like me! Best to err on the side of caution! I’m just illustrating that you don’t need to hit the panic button if you do cut, burn, or bruise yourself. Clean the cut or burn, apply some antiseptic if you have it, and keep an eye on it for signs of infection (redness, soreness, pus etc). If you develop an infection, go straight to your GP for some antibiotics to clear it up quickly, and take the pressure off the lymph system (hence why it is important to have some precautionary antibiotics if you are going to be out of reach of western medicine for a while).
What are the symptoms of lymphoedema developing?
The main symptoms are:
- Swelling – either noticeable swelling compared to your non-BC arm, or if your watch, rings or clothes suddenly feel tighter.
- Change in feeling of the arm. This could be pain, aching, heavy-feeling, tightness or stiffness. Please note that surgery itself causes these symptoms, but best to get any weird feelings checked out…just in case.
- Changes in skin texture. This could be dryness, flakiness, tightness of the skin feeling stretched or an orange-peel effect.
If you develop any of these, book in to see your GP, breast care nurse, lymphoedema nurse or surgeon ASAP. Again, they don’t necessarily mean you have developed it – it could be down to something like cellulitis or a blood clot – but whatever it is, you want to get it sorted!
How do you treat lymphoedema?
The main treatments are below.
- Compression sleeve and gauntlet. You will be fitted for a lymphoedema sleeve and glove which compresses the tissue to stop the fluid from building up.

- Manual lymphatic drainage (MLD). This is a form of massage performed by an experienced therapist which encourages the lymph fluid to move away from the swollen tissue so it can drain away.
- Simple lymphatic drainage (SLD). This is a simpler form of the MLD – which you are taught to do yourself at home.
For more information please see the Macmillan website, Breast Cancer Care website or The Lymphoedema Support Network website.
So far, I have been lucky, but know quite a few ladies who haven’t been quite so fortunate and developed lymphoedema pretty soon after their surgery. A few of them have kindly allowed me to share their experiences and advice:
“I have it in my upper arm which is mildly swollen permanently and never really went down after the post-op swelling. My chest wall also has LD. The swelling is a pain – sometimes my hand gets enormous and looks deformed. The swelling does go up and down but never back to normal. When it aches, I have to put the compression sleeve and glove on as I know that it will swell up shortly afterwards. It’s a mildly sickening ache. The NHS sleeves are in a zombie-flesh colour. The arm and sleeve are different colours of zombie-flesh so look odd. I don’t have to wear the sleeve/glove constantly but am meant to wear it if it is aching or swollen and before any exercise, including housework and driving. It aches horribly when driving, even with the gear on.
I have MLD from the LD nurse every few weeks and she has taught me some simple strokes to do at home. Mine is classified as “mild” even though my hand can swell to twice the size.
With regards everyday life, I have to be careful with which clothes to wear – both to cover up my sleeve and the swelling and also to ensure that they are not too tight or restrictive. The compression sleeve can also be uncomfortable and can chafe. It’s also a bugger when washing hands! The glove has to come off and the sleeve’s hand-anchor has to be rolled back. The glove also gets very grubby very quickly.”
—
“The first indication I had was a heavy feeling in my arm and hand with no obvious change in size. My arm would ache and it was more annoying than sore. I was a right-sided node clearance and right-handed so the more active I became after treatment the more I realised there was a potential risk of lymphoedema as my hand felt tight and would swell at night. However the trigger was when my hand ballooned while I was decorating. The main trigger for me is using it too much – I therefore wear a glove and sleeve when I do specific tasks like housework, writing and decorating. I wear it to work as I’m office based and typing triggers it off. Luckily I caught mine before it took hold so to speak and I can control it. Prevention is better than a cure. If anyone suspects they have it, it must be checked ASAP. The sleeves and gloves are provided in nude (yuck) however I now have a couple of black sets which people strangely don’t notice as much . Mine mainly affects my hand , but my arm can swell too.
So the main symptoms for me was a heavy, achy arm , then tightness and swelling at night and lastly the ballooned hand when using it too much. I only wear the sleeve when at work and occasionally at home. I can play on it at home to avoid nasty tasks!!!!!”
—
“My lymphoedema started 3 months ago, almost as soon as rads had finished. Mine is in my breast which is very swollen, red and hot, and the skin all over breast is like orange peel. I am told by specialist that this is the first classic sign of LD. The pain is a constant throbbing with shooting pains that travel all the way down to fingertips. I wear a crop top style sports bra as it supports it well and feels more comfortable with it on.”
—
“Remember American Tan tights? Welcome to the world of American Tan arms. As there are different makes and sizes, it can be a question of trial and error to find a sleeve that fits without pinching while still giving the right sort of compression. Manual lymphatic drainage (MLD) can be REALLY helpful, but it can be a bit of a lottery for how often you can get it on the NHS. In the meantime, you can do Self Lymphatic Drainage (SLD). For best results get into the habit of doing this regularly, to keep the lymphoedema under as much control as possible.
Something else to watch out for if you have lymphoedema is any scratches or insect bites, which could result in cellulitis, a very painful inflammation of the tissue in the affected area. A useful tip is to keep a travel tube of antiseptic cream or wipes with you wherever you go, in case you do get scratched.
If you have lymphoedema in the hands, you may need to wear the rather sexy gauntlets. Unfortunately, they can get dirty quickly, so get hold of a box of latex gloves (if you’re not allergic to latex, of course) to keep in the kitchen, and shove a few in your bag too, in case you do anything messy when out and about. Use them whenever you’re preparing food, eating anything messy or sticky, and when using the loo.”
—
Thanks girls! If you are really not getting on with the tan compression sleeve, you can ask your GP or LD nurse to prescribe you a black one (some will, some wont – and some chemists wont dispense them) or buy an alternative sleeve or cover. You can buy patterned covers like My Tattoo Sleeve online. There are many more companies in the States that do sleeve covers and coloured and patterned lymphoedema sleeves – but be wary if you are buying an actual sleeve as you need to make sure that it fits your personal prescription and size.
Tags: Breast Cancer, lymphoedema, lymphoedema sleeve
 It is a bit of a work in progress and I will be updating it daily over the next few weeks, so please bear with me.
It is a bit of a work in progress and I will be updating it daily over the next few weeks, so please bear with me.